Key Takeaways:
- Regular blood sugar logging helps you and your healthcare provider manage diabetes effectively.
- Our printable blood sugar log lets you easily track your blood glucose levels.
- Continuous glucose monitors through your insurance and Aeroflow Diabetes offer a convenient, comprehensive way to monitor blood sugar.
Blood glucose monitoring is an essential part of life for those who take insulin to manage type 1 or type 2 diabetes, and it’s the primary way to tell if your blood sugar levels are within the target range.
For people with diabetes who measure their glucose levels several times a day with a blood glucose meter, a blood sugar log is an invaluable tool. Get a free printable blood sugar log sheet and keep track of your health!
Benefits of Using a Blood Sugar Log Sheet
By consistently recording and reviewing your blood sugar levels, you and your healthcare provider can identify patterns and develop an effective diabetes care plan.
Over time, this plan can be improved based on how your blood sugar responds to food, medication, and physical activity.
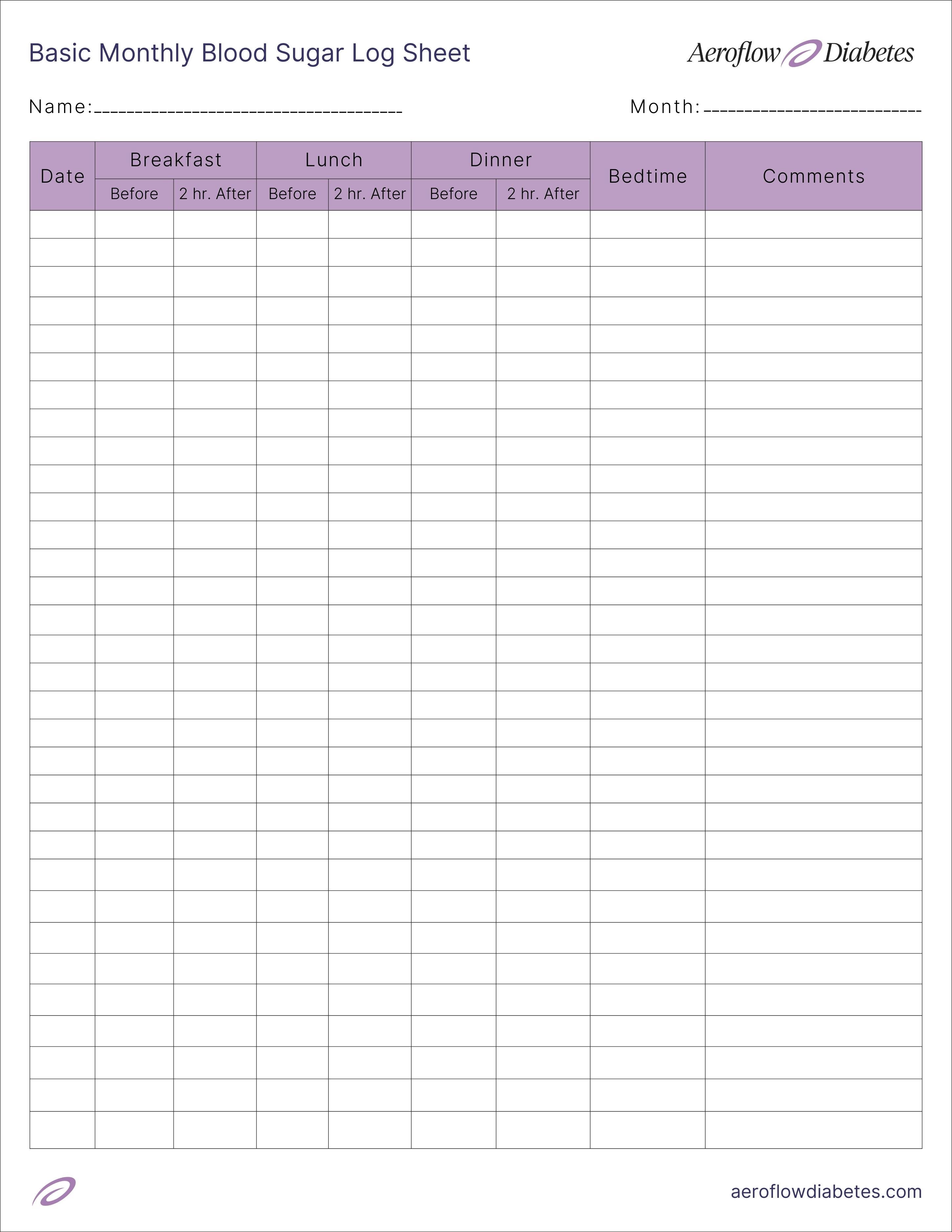
Free Printable Blood Sugar Log Sheet
We’ve developed a free blood sugar log sheet to make record-keeping easier. Download the sheet now to start tracking your diabetes management.
How to Use Your Blood Sugar Log Sheet
To use this blood glucose log effectively, follow these steps.
- Record your blood glucose levels before and two hours after each meal and at bedtime.
- In the comments section, note any other factors that may have affected your blood sugar levels, including stress or physical activity.
- For access to other detailed diabetes log templates that record insulin doses, carbs consumed, and other variables, consult the Johns Hopkins Patient Guide to Diabetes.
Check your coverage for continuous glucose monitoring supplies through your insurance now!
Check your coverage for continuous glucose monitoring supplies through your insurance now!
Blood Sugar Level Recommendations
Your blood sugar levels may change as you go about your daily routines.
- Before a meal: The American Diabetes Association recommends that pre-meal blood sugar levels be between 80 and 130 mg/dL for most non-pregnant adults with diabetes.
- After a meal: The recommendation for blood sugar level measured one to two hours after a meal is less than 180 mg/dL.
These target ranges may need to be adjusted for individuals based on age, cardiovascular health, duration of diabetes, and other factors.
It’s essential to speak with your healthcare provider to determine your optimal target ranges.
Get Continuous Glucose Monitors at Low Cost
If you have type 1 diabetes, take insulin or use an insulin pump, check your blood glucose levels several times a day, and require frequent adjustment to your insulin dose, your health insurance plan may help cover the cost of a continuous glucose monitoring (CGM) device.
A modern alternative to traditional blood glucose meters, CGM devices don’t require painful fingersticks. Instead, they rely on a small sensor implanted just below the skin to measure and report blood glucose levels every few minutes. This type of system produces many more blood sugar readings than a blood glucose meter and can help provide you and your healthcare team with a complete picture of your health.
Using a CGM is also much more straightforward than creating a glucose logbook by hand. It lets you digitally store your blood glucose data and easily share it with your healthcare provider!
If you’re interested in transitioning from a blood glucose meter to a CGM system, the first step is to consult with your healthcare provider. Only they can advise whether you would benefit from a CGM device and if you meet the requirements for insurance coverage.
Aeroflow Diabetes can work directly with your provider and Medicare or private insurance plan to ensure you receive maximum benefits. Currently, we offer both the Dexcom and Freestyle Libre Systems devices, which are all eligible for coverage through insurance.
Complete our easy Eligibility Form today to get started!
Disclaimer
Information provided on the Aeroflow Diabetes blog is not intended as a substitute to medical advice or care. Aeroflow Diabetes recommends consulting a doctor if you are experiencing medical issues or concerns.