Key Takeaways:
- Regular check-ups, education, and a balanced diet are essential for controlling diabetes and preventing complications.
- Lifestyle changes like incorporating exercise, stress management, and healthy eating habits can significantly improve blood sugar levels and overall well-being.
- Utilizing continuous glucose monitors (CGMs) can simplify blood sugar monitoring, making it easier to manage diabetes and maintain a healthy lifestyle.
November is National Diabetes Month, but diabetes is a chronic health condition that demands attention, care, and mindful choices all year round. While managing your condition can be complex, it doesn't have to define your life! In fact, keeping your diabetes in check can result in positive changes that can improve your quality of life by making you healthier.
Whether you're a newly diagnosed diabetic or someone who has been living with diabetes for a long time, this article can serve as a guide to simplify your management routine so you can enjoy life to the fullest.
The Importance of Diabetes Management
According to the American Diabetes Association, about 37.3 million Americans have diabetes. In 2010, only 19% of people with diabetes met management expectations of controlling their blood sugar, blood pressure, and cholesterol levels.
It's vital that you manage diabetes correctly because if it does go unmanaged, it can lead to diabetes complications, such as:
- Hyperglycemia
- Stroke
- Low blood sugar or high blood sugar.
- Heart attack.
- Diabetic ketoacidosis or ketoacidosis coma.
- Nerve damage.
- Hospitalization
- Kidney damage.
- Eye damage.
- Amputation
In the long term, poorly controlled diabetes can lead to complications with several organs, particularly the kidneys, eyes, and nervous system. In addition, the risk of cardiovascular complications such as heart attack and stroke also increases.
Educate Yourself on Managing Your Diabetes
The first step to living with diabetes successfully and safely is learning as much as possible about your condition. Diabetes education may take a little time, but the more you know, the more easily you can manage symptoms. Let's start with some basic information about how your body uses the food you eat for energy and how that food can affect diabetes.
Some foods you eat, such as carbohydrates, get turned into glucose, which is used to fuel your body or stored and used as energy later on. Glucose is managed by insulin, which is a hormone that is usually naturally produced in your pancreas. Insulin helps glucose turn into energy or be stored for later use in your liver or muscle tissues.
Diabetes occurs in people whose bodies can't manage or make the proper amount of insulin, resulting in 2 types of diabetes.
Who Is at Risk?
According to the Centers for Disease Control and Prevention (CDC), it is not as clear why people develop type 1 diabetes compared to type 2.
People who are at risk for developing type 1 diabetes include:
- Those with a family history of type 1 diabetes.
- Children, teens, and young adults.
Those who are at risk for developing type 2 diabetes include:
- People who have pre-diabetes.
- People ages 45 and up.
- Those living with obesity.
- Family history of type 2 diabetes.
- People living a sedentary lifestyle.
- Those who develop gestational diabetes.
- People with fatty liver disease.
Around 5% of people with diabetes have type 1, which usually develops more in children or adolescents than in adults. With type 1 diabetes, your body's immune system attacks the cells that make insulin, causing an autoimmune disease. This attack on the insulin-producing cells results in your body no longer having insulin in the system, making your body unable to process the sugars you eat. These sugars remain in your blood, and your cells starve, causing unregulated blood glucose levels.
Type 1 diabetes requires insulin therapy, which involves injecting insulin into your body throughout the day to avoid high blood sugar levels that can cause nerve, kidney, eye, and heart damage, among other things.
Around 90% of people with diabetes have type 2 diabetes, also known as adult-onset diabetes. When you have type 2 diabetes, your body can make insulin, but your body has insulin resistance, causing unregulated blood glucose levels. Type 2 diabetes usually develops in people who are over 35, overweight, or who don't get enough physical activity.
Type 2 diabetes is treated with lifestyle changes like exercise, a healthy diet, weight management, and sometimes, insulin injections.
Visit Your Healthcare Provider
Whether you have type 1 or type 2 diabetes, regular check-ups are critical for your diabetes care plan. Find a healthcare provider and visit them routinely and during times of uncertainty, including insulin stacking incidents or if you're having pain in your body related to diabetes. It's recommended that people who inject insulin see their healthcare provider every 3 to 4 months, and people who don't inject insulin see their doctor every 4 to 6 months.
What to Include at Check-Ups:
- A1C test: Measures your blood sugar levels over the past 3 months. A1C tests can help you screen for pre-diabetes and diabetes development and help you manage your diabetes overall. You should get this test a minimum number of 2 times per year.
- Foot exam: Used to check for foot problems. During a foot exam, your provider will check for tingling, numbness, ulcers, swelling, or difficulty walking. Foot exams can help prevent future complications with your feet. You should get a foot exam at least once a year.
- Eye exam: Used to check for eye damage related to diabetes by dilating the eyes and looking for retinal damage. Signs of eye damage can help determine the severity of your diabetes. Get an eye exam once a year.
- Kidney screening: Uses blood and urine tests to check your kidneys for diabetic symptoms. Kidney screenings can check how well your kidneys filter your blood and detect chronic kidney disease (CKD). You should get a kidney screening at least once a year.
- Blood pressure check: Measures your blood pressure to detect the risk of stroke or heart attacks. Get a blood pressure check every time you visit your healthcare provider.
- Electrocardiogram: Checks your overall heart function and health and can help prevent heart attacks. Get an electrocardiogram if you're over 50 and have diabetes.
- Dental exam: Examines the gums for gum disease related to diabetes. Get a dental exam every six months.
- Cholesterol test: Checks your cholesterol levels to prevent heart attack, heart disease, or stroke. Have a cholesterol test once a year.
Eat a Balanced Diet
Healthy eating is another excellent step toward developing a beneficial treatment plan, especially if you have type 2 diabetes, since it can be managed with the right food choices. In addition, eating right can help you control your cholesterol, blood pressure, and blood glucose levels, maintain a healthy weight, and prevent diabetes symptoms.
Foods to Eat
- Vegetables
- Fresh fruits.
- Lean proteins, especially fish with Omega-3s.
- Olive oil.
- Nuts and seeds.
- Whole grains.
Foods to Avoid
- Fried foods.
- Foods that contain high levels of salt (sodium).
- Foods with high amounts of sugar, such as sweets.
- Soda
- Fruit juice.
- Other sugary drinks, such as sports drinks.
While you should aim to eat healthy foods, there are ways to eat less healthy foods, like fast food, as long as you plan accordingly. Another helpful tip is using diabetes-friendly shopping lists at the grocery store.
When to Eat
If you have diabetes, it can be tricky to plan your meal times since you may need to base your insulin doses on the food you put into your body. Depending on which type of diabetes you have and what medications you're on, you might need to eat at the same time each day. The most important step in figuring out when to eat is to speak with a healthcare professional to make a diabetes care plan. Then, keep a food log so you know when to inject insulin to avoid insulin stacking or hypoglycemia. Your healthcare provider can also tell you how much you should eat and what foods to include.
Exercise Regularly
Exercise can help lower your blood pressure and blood glucose levels, aid in weight loss, and prevent other health problems. It's important to note that if you inject insulin or take other diabetes medications, you may experience hypoglycemia after exercising. Speak with your healthcare provider about when to eat or take insulin to prevent your blood glucose levels from dropping too low from exercise. You should engage in physical activity at least 3 to 4 times weekly for at least 20-30 minutes per session.
Exercise for Diabetes
- Resistance band exercises.
- Walking
- Cycling
- Swimming
- Weight lifting.
Use Continuous Glucose Monitors
Monitoring your blood sugar levels at home is another excellent part of diabetes self-care, especially if you inject insulin. One of the easiest ways to do this is with the help of a continuous glucose monitor (CGM).
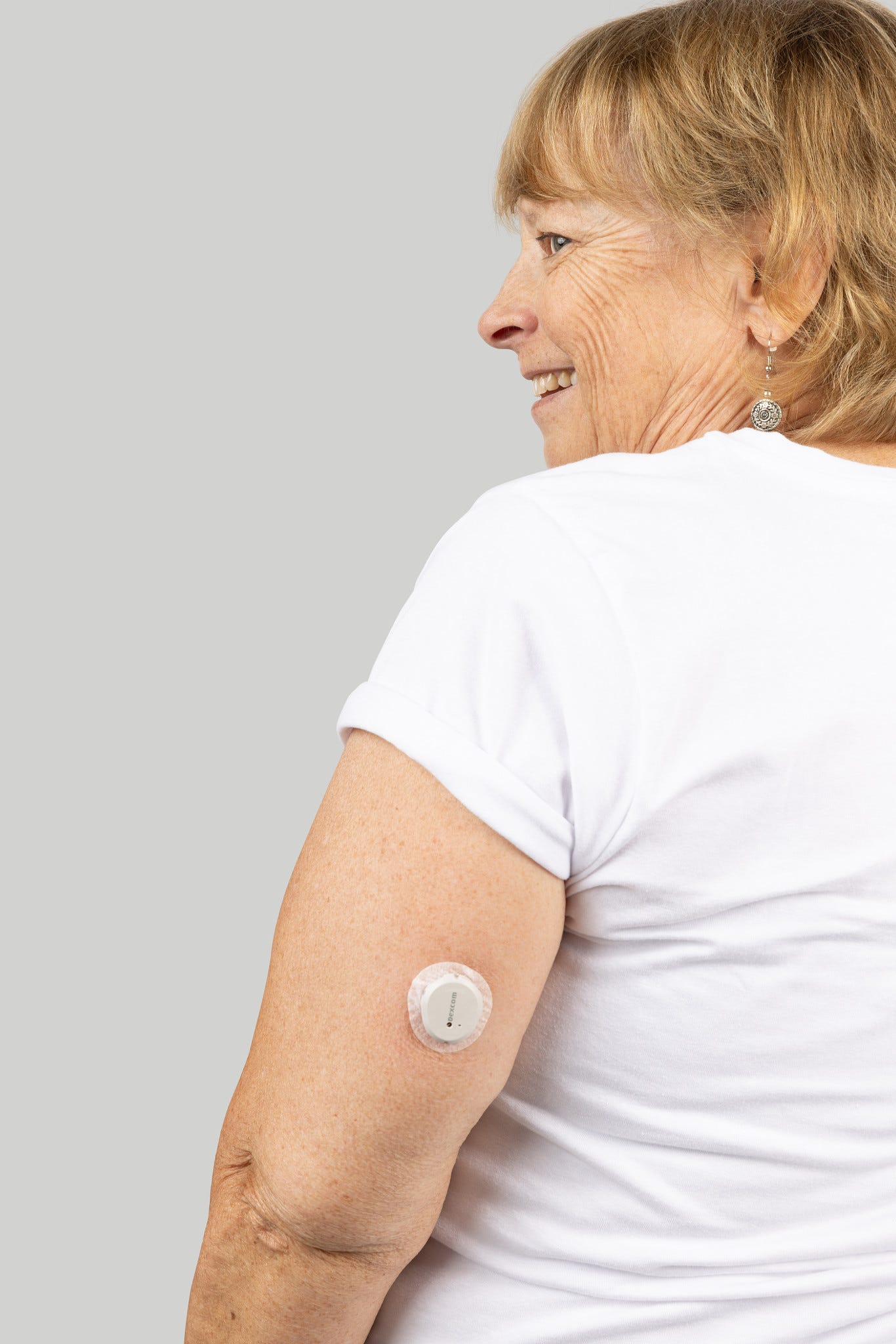
CGMs can easily monitor your glucose levels without using fingerpricks. Instead, the systems work by scanning the interstitial fluid in your body through your skin, usually through a sensor placed on the back of your arm. The sensor then sends information to a transmitter, which sends the data to a portable reader or phone.
CGMs can cost up to $6,000 per year, but Aeroflow Diabetes may be able to supply you with one at little-to-no cost through your Medicare or other insurance plans. To see if you qualify, all you need to do is fill out our Eligibility Form.
If you do qualify, our Diabetes Care Specialists will reach out to you and help you fill out the necessary paperwork from your doctor. They'll also answer any questions you have about the CGMs we offer and any questions you may have about your insurance coverage and costs. Then, you'll choose your supplies, and they'll be shipped directly to your home for free, making your diabetes management more accessible than ever.

Make Lifestyle Changes
The following strategies can help you be more confident in your diabetes self-management plan.
Managing stress can help reduce your blood pressure and increase your mental health. To manage stress, try exercising or engaging in calming activities such as:
- Meditation
- Deep breathing.
- Connecting with others for support.
It's been shown that poor sleep can negatively impact your blood sugar levels, so try to get around 7 to 8 hours of sleep per night.
Drinking enough water has been shown to control your blood sugar levels. Women should drink around 11 cups of water daily, and men should drink about 15 cups.
Obesity is linked to diabetes, so keeping your weight at a healthy level can help manage your symptoms and even prevent diabetes. Talk to your healthcare provider about your ideal weight and how you can stay in the healthy range for your body.
There are specific vitamins that can help you manage diabetes, including:
- Vitamin D.
- Magnesium
- Chromium
- Probiotics
- Certain spices, such as cinnamon.
Get CGMs With Medicare & Aeroflow Diabetes
If you need a CGM to manage your blood glucose levels at home, Aeroflow Diabetes may be able to provide you with one at a low cost through your Medicare or other insurance plan.
To see if you qualify, complete our Eligibility Form.
If you're eligible, a Diabetes Care Specialist will contact you to inform you of the next steps to getting your CGM delivered straight to your home.
References
What is Diabetes? (n.d.). Www.diabetesresearch.org. https://www.diabetesresearch.org/what-is-diabetes#:~:text=Diabetes%20occurs%20when%20your%20body
CDC. (2019). Diabetes Risk Factors. Centers for Disease Control and Prevention. https://www.cdc.gov/diabetes/basics/risk-factors.html
Your Diabetes Care Team. (n.d.). WebMD. Retrieved May 17, 2022, from https://www.webmd.com/diabetes/diabetes-health-care-team#:~:text=come%20with%20diabetes.-
Statistics About Diabetes | ADA. (n.d.). Www.diabetes.org. https://www.diabetes.org/about-us/statistics/about-diabetes#:~:text=Overall%20numbers
More Americans Successfully Managing Diabetes. (n.d.). WebMD. Retrieved May 17, 2022, from https://www.webmd.com/diabetes/news/20130215/more-americans-successfully-managing-diabetes
Aeroflow Diabetes Disclaimer
Information provided on the Aeroflow Diabetes website is not intended as a substitute for medical advice or care from a healthcare professional. Aeroflow recommends consulting your healthcare provider if you are experiencing medical issues relating to diabetes care.










