Key Takeaways:
- As of 2024, approximately 2 million Medicare beneficiaries are utilizing CGMs, and you could be eligible for coverage under the new policy.
- Using a CGM can significantly enhance diabetes management by providing real-time glucose tracking and enabling timely adjustments in treatment.
- Medicare beneficiaries may qualify to receive their CGM at low-cost through insurance with Aeroflow Diabetes.
As of 2024, it’s estimated that around 2 million Medicare beneficiaries use CGMs, and you may also be eligible under the new policy! Use this article to find out if you meet the eligibility requirements and find out how to get a CGM covered by insurance.
Why Should You Get a CGM?
Using a continuous glucose monitor (CGM) can revolutionize diabetes management by offering immediate insights into blood sugar levels without frequent fingersticks. CGMs provide ongoing glucose tracking, revealing trends and patterns that might be missed with the usual periodic testing.
This continuous data stream allows you or a caregiver to review and make timely adjustments in diet, activity, and medication, leading to more precise diabetes management. Enhanced monitoring can significantly improve overall diabetes care by enabling proactive and informed decisions about daily health routines.
New CGM Coverage Policy Explained
In 2024, Medicare policies for CGMs have undergone significant changes to improve access and affordability for beneficiaries. These updates include expanding coverage criteria to encompass a broader range of diabetes management needs, simplifying the qualification process, and reducing out-of-pocket costs.
Additionally, Medicare now covers more advanced CGM models, ensuring beneficiaries have access to the latest technology for an optimal diabetes treatment plan. These changes reflect Medicare's commitment to enhancing the quality of care for individuals with diabetes, promoting better health outcomes, and supporting the use of cutting-edge medical devices.
Under the new CMS guidelines, a person with diabetes simply needs to:
- Be insulin treated rather than use insulin at least 3 times per day OR
- Have a history of "problematic hypoglycemia.”
According to the CMS policy, a person with a “history of problematic hypoglycemia” means you:
- Have at least 2 Level 2 hypoglycemic events with at least 2 previous medication adjustments to your diabetes treatment plan.
- Have at least 1 Level 3 hypoglycemic event with documented proof from a healthcare provider that you required assistance for treatment.
The new policy also states that your healthcare provider must:
- Prove that you have gotten training in the use of CGMs as evidenced by a prescription.
- Prove that your CGM prescription aligns with the Food and Drug Administration (FDA) indications for use.
Because these policies are set forth by Medicare, Aeroflow Diabetes must strictly comply with these guidelines to provide consistent and accurate Medicare coverage. For additional information about policies or Medicare in general, visit medicare.gov.
What Does the New CGM Coverage Policy Mean for Me?
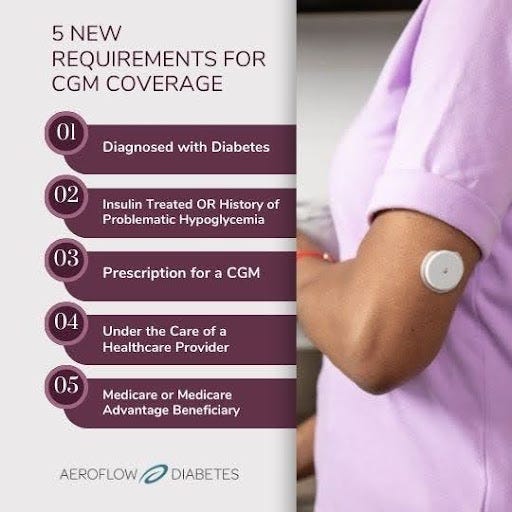
The new Medicare coverage guidelines mean you may qualify for a CGM through your insurance plan. Your coverage determination is based on:
- Having type 1 or type 2 diabetes.
- Being insulin treated and / or have a history of problematic hypoglycemia.
- Being prescribed a CGM by a healthcare provider.
- Being under the care of a healthcare provider.
- Being on a traditional Medicare or Medicare Advantage plan.

Medicare coverage for the latest CGM models ensures that beneficiaries can utilize state-of-the-art devices for accurate and convenient blood glucose monitoring.
Overall, these changes enhance the quality of care, support better health outcomes, and reflect Medicare's commitment to leveraging technology for improved healthcare.
How to Get a CGM Through Medicare & Aeroflow Diabetes
If you meet the new criteria for CGM coverage, the next step is to find a durable medical equipment supplier of insurance-covered CGM devices, like Aeroflow Diabetes! To qualify, it’s required that you’ve had an in-person visit with your healthcare provider within the last 6 months. Medicare-approved telehealth visits are accepted at any location in the U.S., including your home, until the end of 2024. After that, you must be in an office or medical facility located in a rural area to get most telehealth services.
We strive to help you obtain the CGM products you need to live a healthier, happier lifestyle while managing diabetes confidently. Our team will assist you with navigating the updated Medicare policies and ensuring you meet the qualification criteria. We provide personalized guidance to help you manage the process smoothly. Additionally, we offer ongoing support and education to ensure you make the most of your CGM for effective diabetes management.
We make getting a low-cost CGM as simple as possible by:


- Taking care of the confusing insurance paperwork for you and determining your eligibility within 1-2 business days.
- Helping you set up everything in the comfort of your own home by using an easy-to-use online ordering portal.
- Shipping your CGM supplies to your doorstep for free 2 day shipping every month.
- Giving you access to expert Diabetes Specialists.
Do You Qualify for a CGM?
To find out if you or your loved one qualifies for a CGM through insurance, simply fill out our secure Qualification Form.
It’s a short process and we never share your information with any third parties. We’ll reach out to you shortly after you submit your information to inform you of your eligibility status.
From there, you can choose from high-quality, insurance-covered CGMs from your mobile device or computer. Depending on your specific insurance plan, you may be able to choose from the following CGMs:
- Dexcom: Dexcom G6 System or Dexcom G7 System.
- Abbott: FreeStyle Libre 2 System, FreeStyle Libre 14 day System.
Be sure to take advantage of the educational resources on our blog to answer common questions that people with diabetes and CGM users have, like where to wear your CGM, how to connect your CGM to your mobile device, and more!
Aeroflow Diabetes Disclaimer
Information provided on the Aeroflow Diabetes website is not intended as a substitute for medical advice or care from a healthcare professional. Aeroflow recommends consulting your healthcare provider if you are experiencing medical issues relating to diabetes care.